
Emergency Medical Minute
1,158 episodes — Page 12 of 24

On the Streets #2: Neurological Deficits
Part 1 of 2: Dr. Adam Graham dishes out the essentials of identifying concerning neurological deficits on the scene, predicting what they mean and how to best care for patients with neurological deficits in the pre-hospital setting. About Dr. Adam Graham: Adam Graham, MD, is a board-certified neurologist with Blue Sky Neurology in Denver. His professional interests include treatment of diseases of the peripheral nerves and muscles, for example ALS, myasthenia gravis and peripheral neuropathy. He works to make EMG procedures as comfortable as possible for patients. Dr. Graham earned his medical degree from Creighton University. He then completed a residency in neurology and a fellowship in neuromuscular medicine and EMG, both at the University of Colorado.

Podcast 548: Adrenal Crisis
Contributor: Nick Tsipis, MD Educational Pearls: Congenital adrenal hyperplasia (CAH) is a group of enzyme deficiencies in the adrenals leading to a deficiency of hormones normally synthesized by the adrenals (mineralocorticoids, glucocorticoids, androgens) 21-hydroxylase is most commonly the deficient enzyme. 21-hydroxylase is needed to produce aldosterone and cortisol, and those with chronic cortisol deficiencies need daily steroid replacement Aldosterone, made in the kidney as part of the renin-angiotensin-aldosterone system (RAAS), increases blood pressure via salt and water retention to maintain adequate organ perfusion Adrenal crisis results in a loss of cortisol leading to hypoglycemia and potential CNS depression with hypotension, hypoglycemia, and hyponatremia Patients in adrenal crisis need salt, volume, and glucose replacement References Martin-Grace, J., et al. Adrenal insufficiency: physiology, clinical presentation and diagnostic challenges. Clin Chim Acta. 2020 Feb 6. Dineen, R., Thompson, C.J., Sherlock, M. Adrenal crisis: prevention and management in adult patients. Ther Adv Endocrinol Metab. 2019 Jun 13;10:2042018819848218. El-Maouche, D., Arlt, W., Merke, D.P. Congenital Adrenal Hyperplasia. Lancet. 2017 Nov 11;390(10108):2194-2210. Summarized by Jackson Roos, MS3 | Edited by Erik Verzemnieks, MD

Podcast 547: Capsaicin Cream to the Rescue
Author: Aaron Lessen, MD Educational Pearls: A recent retrospective study looked capsaicin cream in treating cannabinoid hyperemesis syndrome in regards to length of stay, cost analysis, use of rescue therapies, and adverse events Results showed a trend towards reduced length of stay but did not reach statistical significance Use of opioids was reduced in the capsaicin group Capsaicin remains a potential treatment option in this often difficult disease References Samantha Wagner, Jason Hoppe, Matthew Zuckerman, Kerry Schwarz & Julie McLaughlin (2019) Efficacy and safety of topical capsaicin for cannabinoid hyperemesis syndrome in the emergency department, Clinical Toxicology, DOI: 10.1080/15563650.2019.1660783 Summarized by Jackson Roos, MS3 | Edited by Erik Verzemnieks, MD

Podcast 546: Complete Heart Block
Author: Jared Scott, MD Educational Pearls: Differentiating symptomatic bradycardia from asymptomatic may be essential in determining workup and treatment Airway, breath, circulation always hold true Symptoms may include dizziness, syncope, or weakness An EKG is essential in the majority of cases Complete heart block can be a cause of symptomatic bradycardia and requires immediate attention Complete heart block can be caused by drugs (beta-blockers, calcium channel blockers), Lyme disease, infiltrative disease, or degeneration of the conduction system References: Kusumoto FM, Schoenfeld MH, Barrett C, Edgerton JR, Ellenbogen KA, Gold MR, Goldschlager NF, Hamilton RM, Joglar JA, Kim RJ, Lee R, Marine JE, McLeod CJ, Oken KR, Patton KK, Pellegrini CN, Selzman KA, Thompson A, Varosy PD. 2018 ACC/AHA/HRS Guideline on the Evaluation and Management of Patients With Bradycardia and Cardiac Conduction Delay: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2019;74(7):e51. Epub 2018 Nov 6. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 545: So You Quit Smoking… Now What?
Author: Aaron Lessen, MD Educational Pearls: New data shows within 5 years of smoking cessation, the risk of cardiovascular disease becomes half of those who continue to smoke After 10-15 years of cessation, cardiovascular disease rates return to rates seen in non-smokers. Lung disease, COPD, and cancer rates do not decrease quite as rapidly, but do decrease It's important to remind patients of the long-term health benefits associated with smoking cessation when counseling them. References Duncan MS, Freiberg MS, Greevy RA, Kundu S, Vasan RS, Tindle HA. Association of Smoking Cessation With Subsequent Risk of Cardiovascular Disease. JAMA. 2019;322(7):642–650. doi:10.1001/jama.2019.10298 Summarized by Jackson Roos, MS3 | Edited by Erik Verzemnieks, MD

UnfilterED #5: Dr. Lisa Zwerdlinger
Recorded remotely in the highest hospital in the world, Nick sits down to talk with Dr. Lisa Zwerdlinger, a small-town physician who's worn many different hats both in the hospital and her community. Intro Music: Backbay Lounge Kevin MacLeod (incompetech.com) Licensed under Creative Commons: By Attribution 3.0 License http://creativecommons.org/licenses/by/3.0/

Podcast 544: C is for Sepsis
Author: Aaron Lessen, MD Educational Pearls: Previously, trials had shown promising evidence that vitamin C may improve mortality rates in patients with sepsis or septic shock. A 2017 retrospective before-after study gave a "cocktail" of hydrocortisone, vitamin C, and thiamine to patients with severe sepsis or in septic shock and reported a decrease in mortality from 40% to 8%. A 2020 randomized controlled trial demonstrated that giving patients hydrocortisone, vitamin C, and thiamine showed no benefits in improving sepsis outcomes. Currently use of Vitamin C in sepsis and septic shock remains controversial due to lack of sufficient data References 1) Marik PE, Khangoora V, Rivera R, Hooper MH, Catravas J. Hydrocortisone, Vitamin C, and Thiamine for the Treatment of Severe Sepsis and Septic Shock: A Retrospective Before-After Study. Chest. 2017;151(6):1229. Epub 2016 Dec 6. 2) Fujii T, Luethi N, Young PJ, et al. Effect of Vitamin C, Hydrocortisone, and Thiamine vs Hydrocortisone Alone on Time Alive and Free of Vasopressor Support Among Patients With Septic Shock: The VITAMINS Randomized Clinical Trial. JAMA. 2020;323(5):423–431. doi:10.1001/jama.2019.22176 Summarized by Jackson Roos, MS3 | Edited by Erik Verzemnieks, MD

Podcast 543: Scoring Blunt Traumatic Aortic Injury
Author: Nick Tsipis, MD Educational Pearls: Aortic injury caused by blunt trauma is very rare Chest x-ray findings might include widening of the mediastinum Ligamentum arteriosum (remnant of the ductus arteriosus) tethers the aorta to the chest wall, potentially causing injury with abrupt decelerations and motion XR lacks significant sensitivity (around 75%) to be utilized in many cases CT angiogram (CTA) of the chest is typically the preferred test but comes with potential risks including radiation exposure NEXUS Decision Instrument (NEXUS DI) is a scoring tool that may provide value in determining the need for additional imaging References Yu L, Baumann BM, Raja AS, Mower WR, Langdorf MI, Medak AJ, Anglin DR, Hendey GW, Nishijima D, Rodriguez RM. Blunt Traumatic Aortic Injury in the Pan-scan Era. Acad Emerg Med. 2019 Dec 7. doi: 10.1111/acem.13900. Summarized and edited by Erik Verzemnieks, MD

Mental Health Monthly #2: Non-Epileptic Seizures (NES)
Non Epileptic Seizures (NES) is perhaps one of the most misunderstood and overlooked disorders that emergency medicine professionals encounter. Dr. Randi Libbon & Dr. Laura Strom, both experts on NES, explain the ongoing research surrounding the topic as well as how to best manage patients with NES in the emergency setting. To learn more about Dr. Randi Libbon: https://www.cudoctors.com/Find_A_Doctor/Profile/25375 To learn more about Dr. Laura Strom: http://www.ucdenver.edu/academics/colleges/medicalschool/departments/neurology/Faculty/Pages/Strom.aspx References & Further Reading: [1] Baslet G, Seshadri A, Bermeo-Ovalle A, Willment K, Myers L. Psychogenic Non-epileptic Seizures: An Updated Primer. Psychosomatics. 2016;57(1):1-17. doi:10.1016/j.psym.2015.10.004 [2] Perez DL, LaFrance WC. Nonepileptic Seizures: An Updated Review. CNS Spectr. 2016;21(3):239-246. doi:10.1017/S109285291600002X [3] Libbon R, Gadbaw J, Watson M, et al. The feasibility of a multidisciplinary group therapy clinic for the treatment of nonepileptic seizures. Epilepsy Behav. 2019;98:117-123. doi:10.1016/j.yebeh.2019.06.032 [4] Ding J-R, An D, Liao W, et al. Altered Functional and Structural Connectivity Networks in Psychogenic Non-Epileptic Seizures. PLoS ONE. 2013;8(5). doi:10.1371/journal.pone.0063850 [5] Allendorfer JB, Nenert R, Hernando KA, et al. FMRI response to acute psychological stress differentiates patients with psychogenic non-epileptic seizures from healthy controls – A biochemical and neuroimaging biomarker study. NeuroImage Clin. 2019;24:101967. doi:10.1016/j.nicl.2019.101967
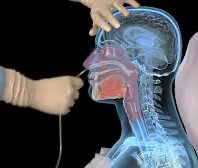
Podcast 542: Nasogastric Tubes
Author: Don Stader, MD Educational Pearls: Nasogastric tubes (NGT) are very uncomfortable for all those involved but some simple tricks and tips may help: Topical lidocaine can be inserted into the nasal passage for local analgesia Afrin may help shrink the mucosal tissue of the nasal turbinates as well Molding the tube with cold/ice water can help - putting it in an ice bath with an endotracheal tube stylet will allow you to mold the tip to your preference References Lor YC, Shih PC, Chen HH, et al. The application of lidocaine to alleviate the discomfort of nasogastric tube insertion: A systematic review and meta-analysis. Medicine (Baltimore). 2018;97(5):e9746. doi:10.1097/MD.0000000000009746 https://www.acepnow.com/article/making-ng-tube-placement-less-horrendous/ https://www.aliem.com/trick-of-trade-making-ng-and-np-painless/ Summarized and edited by Erik Verzemnieks, MD

Podcast 541: Needle Thoracostomy
Author: Aaron Lessen, MD Educational Pearls: Traditional technique of needle thoracostomy for tension penumothorax is along the 2nd intercostal space at the midclavicular line Inserting a large angiocatheter along the 4th or 5th intercostal space at the mid-axillary line may provide a thinner area that is more easily identified, overcoming many of the obstacles of the traditional approach The 10th Edition of ATLS now recommends this location as well A finger thoracostomy, where a scalpel and then the finger are used to penetrate the pleural cavity at the same location, is another method to provide quick decompression of a traumatic tension pneumothorax, allowing a tube thoracostomy to be performed later References Laan DV, Vu TD, Thiels CA, et al. Chest wall thickness and decompression failure: A systematic review and meta-analysis comparing anatomic locations in needle thoracostomy. Injury. 2016;47(4):797–804. doi:10.1016/j.injury.2015.11.045 Inaba K, Branco BC, Eckstein M, Shatz DV, Martin MJ, Green DJ, Noguchi TT, Demetriades D. Optimal positioning for emergent needle thoracostomy: a cadaver-based study. J Trauma. 2011 Nov;71(5):1099-103; discussion 1103. doi: 10.1097/TA.0b013e31822d9618. Summarized and edited by Erik Verzemnieks, MD

On the Streets #1: The Art of the Handoff Report
EMM is proud to present the pilot episode of our new monthly series, "On the Streets". This will be an informative podcast for all of our listeners, but this one was designed specifically for our EMS listeners. Each month, we will consult medical experts on topics pertinent to prehospital care: Identifying a posterior circulation stroke in the field; Knowing when to do a 12-lead and what to look for; How to use capnography for a variety of datapoints; How to give an effective handoff report. And much much more... On our first episode, we are proud to welcome long-time friend of EMM, now retired Emergency Physician and current Medical Director of the ACC EMS program, Dr. Michael Hunt. This episode focuses exclusively on the Do's and Don'ts of giving handoff report. As we all know, knowledge and timing can make a world of difference when treating acutely ill patients. Like all of our content, we aim to equip you with the resources to forge your medical knowledge while keeping it relevant and time-efficient. Tune into "On the Streets" for real, raw and relevant EMS education. Photo Credit: https://www.flickr.com/photos/sc-axman/2327963351/

Podcast 540: Zyprexa
Contributor: Don Stader, MD Educational Pearls: Olanzapine (Zyprexa) is an atypical antipsychotic that can be used in a similar fashion to haloperidol for pain and nausea, including that with abdominal pain and headaches Olanzapine can be administered as an oral disolving tablets, intramuscular or intravenous injection Because Zyprexa is an atypical antipsychotic, it has a lower risk for tardive dyskinesia and akathisia Olanzapine may cause transient rises in glucose and should be considered when contemplating use in a diabetic References Olanzapine for the prevention and treatment of cancer-related nausea and vomiting in adults.Sutherland A, Naessens K, Plugge E, Ware L, Head K, Burton MJ, Wee B. Cochrane Database Syst Rev. 2018;9:CD012555. Epub 2018 Sep 21. Silberstein, S.D., Peres, M.F., Hopkins, M.M., Shechter, A.L., Young, W.B. and Rozen, T.D. (2002), Olanzapine in the Treatment of Refractory Migraine and Chronic Daily Headache. Headache: The Journal of Head and Face Pain, 42: 515-518. doi:10.1046/j.1526-4610.2002.02126. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD
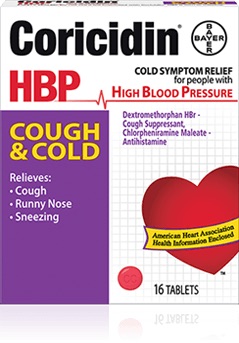
Podcast 539: Coricidin Abuse
Contributor: Rachel Beham, PharmD Educational Pearls: Coricidin HBP Cough & Cold (dextromethorphan and chlorpheniramine) is one of the more commonly abused over-the-counter medications Dextromethorphan, binds to multiple receptors, particularly at high doses Opioid receptors, causing respiratory depression, CNS depression NMDA receptors, causing agitation and hallucinations Serotonin-reuptake inhibition, which may lead to serotonin syndrome, especially when combined with other agents Dextromethorphan also contains bromide, which when chronically abused can lead to bromism (behavioral changes, hallucinations, weight loss, and neurologic changes) Chlorpheniramine is an antihistamine and can cause anticholinergic effects in overdose, such agitation, hyperthermia, and hallucinations Acute treatment of Coricidin abuse is mostly supportive, which may include benzodiazepines, naloxone, dialysis, sodium bicarbonate, and physostigmine depending on the predominate toxidrome and symptoms present References Ritter D, Ouellette L, Sheets JD, Riley B, Judge B, Cook A, Houseman J, Jones JS. "Robo-tripping": Dextromethorphan toxicity and abuse. Am J Emerg Med. 2019 Nov 17. pii: S0735-6757(19)30655-2. doi: 10.1016/j.ajem.2019.10.001. Bryner JK, Wang UK, Hui JW, Bedodo M, MacDougall C, Anderson IB. Dextromethorphan abuse in adolescence: an increasing trend: 1999-2004. Arch Pediatr Adolesc Med. 2006;160(12):1217–1222. doi:10.1001/archpedi.160.12.1217 Monks S, Yen M, Myers J. Bromism: An overlooked and elusive toxidrome from chronic dextromethorphan abuse. Am J Emerg Med. 2019 Nov 15:158491. doi: 10.1016/j.ajem.2019.158491. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 538: Low Maintenance Boxer's Fracture
Contributor: Jared Scott, MD Educational Pearls: A distal 5th metacarpal neck fracture is often referred to as a "boxer's fracture" and a common fracture encountered in the emergency department Splinting with an ulnar gutter splint is the typical management of uncomplicated boxer's fractures A recent study randomized patients to buddy taping or ulnar gutter splint for uncomplicated Boxer's fractures. Similar functional and pain outcomes were found at follow-up, and those in the buddy taping group returned to work more quickly. One limitation was nearly 20% of study patients were lost to follow up Editor's note: remember - this only applies to a true boxer's fracture, which is a distal 5th metacarpal neck fracture, not just any 5th metacarpal shaft fracture References Richard Pellatt, Igor Fomin, Carli Pienaar, Randipsingh Bindra, Michael Thomas, Ezekiel Tan, Cindy Mervin, Ping Zhang, Gerben Keijzers. Is Buddy Taping as Effective as Plaster Immobilization for Adults With an Uncomplicated Neck of Fifth Metacarpal Fracture? A Randomized Controlled Trial, Annals of Emergency Medicine, Volume 74, Issue 1, 2019, Pages 88-97, Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 537: Thoughts on Cardiac Arrest
Contributor: Don Stader, MD Educational Pearls: High-quality compressions are an essential, and probably one of the most important, part of cardiac arrest Actual evidence for drugs in cardiac arrest included in ACLS are limited, including epinephrine, bicarbonate, amiodarone, etc. Early defibrillation for ventricular tachycardia (VT) or ventricular fibrillation (VF) has a plethora of supporting evidence Double-sequential defibrillation (nearly simultaneous defibrillation using 2 machines) may be considered for refractory dysrhythmias like VF tPA during a cardiac arrest can be considered in the setting of massive PE (although the evidence supporting this practice is poor) Ending a cardiac arrest resuscitation is a difficult decision and use of ultrasound may be helpful to assess for meaningful cardiac function/activity References Link MS, Berkow LC, Kudenchuk PJ, Halperin HR, Hess EP, Moitra VK, Neumar RW, O'Neil BJ, Paxton JH, Silvers SM, White RD, Yannopoulos D, Donnino MW . Part 7: Adult Advanced Cardiovascular Life Support: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2015 Nov;132(18 Suppl 2):S444-64. Wang Y, Wang M, Ni Y, Liang B, Liang Z. Can Systemic Thrombolysis Improve Prognosis of Cardiac Arrest Patients During Cardiopulmonary Resuscitation? A Systematic Review and Meta-Analysis.J Emerg Med. 2019;57(4):478. Epub 2019 Oct 5. Eric Cortez, William Krebs, James Davis, David P. Keseg, Ashish R. Panchal. Use of double sequential external defibrillation for refractory ventricular fibrillation during out-of-hospital cardiac arrest. Resuscitation. Volume 108. 2016. Pages 82-86, Atkinson PR, Beckett N, French J, Banerjee A, Fraser J, Lewis D. Does Point-of-care Ultrasound Use Impact Resuscitation Length, Rates of Intervention, and Clinical Outcomes During Cardiac Arrest? A Study from the Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHoC-ED) Investigators. Cureus. 2019;11(4):e4456. Published 2019 Apr 13. doi:10.7759/cureus.4456 Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

UnfilterED #4: Dr. Vivek Tayal
Dr. Vivek Tayal of Carolinas Medical Center, a pioneer of using ultrasound in the emergency department, reflects on his role in establishing ultrasound use in emergency medicine and much more! Ultrasound Program Management: https://www.amazon.com/Ultrasound-Program-Management-Point-Care/dp/3319631411 Intro Music: Backbay Lounge Kevin MacLeod (incompetech.com) Licensed under Creative Commons: By Attribution 3.0 License http://creativecommons.org/licenses/by/3.0/

Podcast 536: Epistaxis 101
Contributor: Dylan Luyten, MD Educational Pearls: Clear the nasal passages - have the patient, if stable, blow their nose to dislodge any clot that might be in the way Searching for the source of bleeding can be tough. Majority of anterior bleeding is from Kesselbach's plexus Placing a clamp to provide direct pressure is a mainstay of treatment Application of a topical agent, which may include lidocaine epinephrine tetracaine (LET), tranexamic acid (TXA), or oxymetazoline Nasal packing with a nasal balloon or merocel may be necessary if bleeding persists Posterior epistaxis can be potentially devastating - for all practical purposes are epistaxis that does not resolve with anterior packing Interventional radiology can be a helpful consultant for controlling of posterior epistaxis, and may be just as or more helpful than ENT References Supriya M, Shakeel M, Veitch D, Ah-See K. Epistaxis: prospective evaluation of bleeding site and its impact on patient outcome. J Laryngol Otol. 2010;124(7):744-749. Shargorodsky J, Bleier B, Holbrook E, et al. Outcomes analysis in epistaxis management: development of a therapeutic algorithm. Otolaryngol Head Neck Surg. 2013;149(3):390-398. Singer A, Blanda M, Cronin K, et al. Comparison of nasal tampons for the treatment of epistaxis in the emergency department: a randomized controlled trial. Ann Emerg Med. 2005;45(2):134-139. Womack JP, Kropa J Jimenez Stabile M. Epistaxis: Outpatient Management. Am Fam Physician. 2018 Aug 15;98(4):240-245. Liu WH, Chen YH, Hsieh CT, Lin EY, Chung TT, Ju DT. Transarterial embolization in the management of life-threatening hemorrhage after maxillofacial trauma: a case report and review of literature. Am J Emerg Med. 2008 May;26(4):516.e3-5. doi: 10.1016/j.ajem.2007.07.036. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 535: A Prescription for Falls
Contributor: Aaron Lessen, MD Educational Pearls: Emergency department evaluation of falls, particularly in the elderly, should include an assessment of risk factors Common causes of falls in the elderly include medications. Review medication list for sedating medications amongst others Consult with your hospital physical therapist to discuss fall prevention techniques with the patient One study has shown that a comprehensive interdisciplinary approach to geriatric falls in the ED can reduce return visits and hospital admissions. References Caplan GA, Williams AJ, Daly B, Abraham K. A randomized, controlled trial of comprehensive geriatric assessment and multidisciplinary intervention after discharge of elderly from the emergency department--the DEED II study. J Am Geriatr Soc. 2004;52(9):1417–23. Albert M, Rui P, McCaig LF. Emergency department visits for injury and illness among adults aged 65 and over: United States, 2012-2013. NCHS Data Brief. 2017;(272):1–8. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Mental Health Monthly #1: Decision Making Capacity
In the first episode of this new series, the complexities of decision making capacity are discussed. References and Further Reading: [1] Appelbaum, P. S. (2007). Assessment of patients' competence to consent to treatment. New England Journal of Medicine, 357(18), 1834-1840. [2] Etchells, E., Darzins, P., Silberfeld, M., Singer, P. A., McKenny, J., Naglie, G., ... & Strang, D. (1999). Assessment of patient capacity to consent to treatment. Journal of general internal medicine, 14(1), 27-34. Joint Centre for Bioethics - Aid to Capacity Evaluation (ACE)

Podcast 534: Nerve Agents
Author: Michael Hunt, MD Educational Pearls: Organophosphate "nerve agents" were developed in the 1930's These agents have cholinergic effects, which can be remembered by the mnemonic "SLUDGE" Salivation Lacrimation Urination Defecation GI cramping Emesis The "SLUDGE" toxidrome is mediated through the muscarinic acetylcholine receptors. Nerve agents also affect the nicotinic acetylcholine receptors, which leads to muscle paralysis Death in these cases is from respiratory collapse due to secretions (bronchorrhea) and diaphragmatic paralysis Treatment includes atropine to reduce secretions (often in incredibly high doses) and pralidoxime (2-PAM) to treat muscle paralysis Benzodiazepines may be necessary for seizures References https://www.osha.gov/SLTC/emergencypreparedness/guides/nerve.html Michael Eddleston Novel Clinical Toxicology and Pharmacology of Organophosphorus Insecticide Self-Poisoning. Annual Review of Pharmacology and Toxicology 2019 59:1, 341-360 Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 533: Hypoglycemia
Contributor: Dylan Luyten, MD Educational Pearls: Insulin related hypoglycemia can vary from a brief transient effect from short-acting forms (i.e. insulin lispro) to prolonged from long acting (i.e. insulin glargine), and will require different treatment and/or observation Of oral glycemic agents, sulfonylureas are a common culprit while metformin is rarely a cause Sulfonylureas also deserve attention because in pediatric patients, they can be lethal even with a single ingestion, but also can cause severe hypoglycemia in adults Hypoglycemia in non-diabetics usually occurs in the malnourished, or in those with liver or adrenal disease References Klein-Schwartz W, Stassinos GL, Isbister GK. Treatment of sulfonylurea and insulin overdose. Br J Clin Pharmacol. 2016;81(3):496–504. doi:10.1111/bcp.12822 Tourkmani AM, Alharbi TJ, Rsheed AMB, AlRasheed AN, AlBattal SM, Abdelhay O, Hassali MA, Alrasheedy AA, Al Harbi NG, Alqahtani A. Hypoglycemia in Type 2 Diabetes Mellitus patients: A review article. Diabetes Metab Syndr. 2018 Sep;12(5):791-794. doi: 10.1016/j.dsx.2018.04.004. Epub 2018 Apr 12. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 532: SVC Syndrome
Contributor: Jared Scott, MD Educational Pearls: Superior vena cava (SVC) syndrome is caused by physical compression of the SVC and can present with facial swelling, upper extremity swelling, flushing, and parasthesias Common causes of SVC syndrome include lung cancer, lymphoma, and thymoma Keep SVC syndrome on the differential for all patients with facial or upper extremity swelling References The superior vena cava syndrome: clinical characteristics and evolving etiology. Rice TW, Rodriguez RM, Light RW. Medicine (Baltimore). 2006;85(1):37. Diagnosis and management of superior vena cava syndrome. Markman M. Cleve Clin J Med. 1999;66(1):59. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 531: Migraine Cocktail
Contributor: Don Stader, MD Educational Pearls: The classic migraine cocktail includes: Reglan (or other dopamine antagonist), Benadryl, Toradol, Decadron, and IV fluids. The most effective agent in the cocktail is a dopaminergic agent Routine IV fluids have not shown efficacy There is no evidence for pre-treatment of akathisia with diphenhydramine (Benadryl) Decadron reduces rebound headache Consider trigger point injections for those with migraine attributable to cervical neck pain. References Jones CW, Remboski LB, Freeze B, Braz VA, Gaughan JP, McLean SA..Intravenous Fluid for the Treatment of Emergency Department Patients With Migraine Headache: A Randomized Controlled Trial. Ann Emerg Med. 2019 Feb;73(2):150-156. doi: 10.1016/j.annemergmed.2018.09.004. Epub 2018 Oct 26. Friedman BW, Cabral L, Adewunmi V, et al. Diphenhydramine as Adjuvant Therapy for Acute Migraine: An Emergency Department-Based Randomized Clinical Trial. Ann Emerg Med. 2016;67(1):32–39.e3. doi:10.1016/j.annemergmed.2015.07.495 Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 530: Anion Gap Acidosis + Metformin Toxicity
EContributor: Don Stader, MD Educational Pearls: The common causes of anion gap metabolic acidosis include (MUDPILES) Metformin, Methanol Uremia DKA Paraldehyde INH/Iron Lactate Ethylene Glycol Salicylate Metformin is a very common drug used to treat type 2 diabetes, however in the right setting, it can cause a profound lactic acidosis. There is a very high mortality rate. Treatment of metformin toxicity includes fluids, bicarb, and dialysis Most commonly, metformin toxicity is in the setting of kidney injury or overdose. Always consider acidosis in those with tachypnea! References Re-evaluation of a biguanide, metformin: mechanism of action and tolerability. Sirtori CR, Pasik C Pharmacol Res. 1994;30(3):187. Bicarbonate haemodialysis as a treatment of metformin overdose.Heaney D, Majid A, Junor B. Nephrol Dial Transplant. 1997;12(5):1046. Extracorporeal Treatment for Metformin Poisoning: Systematic Review and Recommendations From the Extracorporeal Treatments in Poisoning Workgroup.Calello DP, Liu KD, Wiegand TJ, Roberts DM, Lavergne V, Gosselin S, Hoffman RS, Nolin TD, Ghannoum M, Extracorporeal Treatments in Poisoning Workgroup Crit Care Med. 2015;43(8):1716. Metformin accumulation: lactic acidosis and high plasmatic metformin levels in a retrospective case series of 66 patients on chronic therapy.Vecchio S, Giampreti A, Petrolini VM, Lonati D, Protti A, Papa P, Rognoni C, Valli A, Rocchi L, Rolandi L, Manzo L, Locatelli CA Clin Toxicol (Phila). 2014;52(2):129. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD
Podcast 529: Hemophilia
Contributor: Aaron Lessen, MD Educational Pearls: Hemophilia is characterized by bleeding (A /B) A is is 8, B (chrstmas, 9) Hemophilia refers to a group of bleeding disorders caused by a deficiency in a certain clotting factor. The two most common are hemophilia A (caused by a lack of factor VIII), and B (caused by a lack of factor 9) Most cases are inherited in an X-linked recessive manner. Therefore, males are the most commonly affected. However, spontaneous cases do occur in all sexes. People with hemophilia can present to the ED with a variety of bleeding complications including hemarthrosis, intracranial hemorrhage, and GI bleeds. Treatment is guided by the type of hemophilia and the degree of bleeding, with the most severe cases being treated with replacement of 100% of that person's deficient clotting factor. Timely treatment improves outcomes, so consider empiric therapy in those with known hemophilia References Hemophilia A in the third millennium.Franchini M, Mannucci PM Blood Rev. 2013 Jul;27(4):179-84. Epub 2013 Jun 28. Rheumatic manifestations of hematologic disorders.Aviña-Zubieta JA, Galindo-Rodriguez G, Lavalle C Curr Opin Rheumatol. 1998;10(1):86. The molecular genetics of hemophilia: blood clotting factors VIII and IX.Lawn RM Cell. 1985;42(2):405. Guidelines for the management of hemophilia.Srivastava A, Brewer AK, Mauser-Bunschoten EP, Key NS, Kitchen S, Llinas A, Ludlam CA, Mahlangu JN, Mulder K, Poon MC, Street A, Treatment Guidelines Working Group on Behalf of The World Federation Of Hemophilia Haemophilia. 2013 Jan;19(1):e1-47. Epub 2012 Jul 6. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD
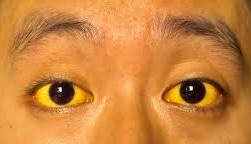
Podcast 528: Decompensated Liver Failure
Contributor: Michael Hunt, MD Educational Pearls: Cirrhosis is the end stage of chronic structural damage to the liver. This is most commonly due to alcohol but other causes viral hepatitis and hepatotoxic drugs Cirrhotic patients are very prone to GI bleeding and infections, partially due to the role the liver plays in producing immune and clotting factors These patients can easily become "sick". Use the shock index (heart rate / systolic blood pressure) as a rapid assessment of hemodynamic status. >0.7 is worrisome, >1 should prompt resuscitation. Because cirrhotic patients are immunocompromised, do not rely on the presence of fever and peritonitis to diagnose spontaneous bacterial peritonitis (SBP), and have a low threshold to perform a diagnostic paracentesis Polymorphonuclear (PMN) count > 250 in the ascitic fluid suggests SBP With GI bleeding in cirrhotics, antibiotics have a mortality benefit, while PPIs and octreotide have limited benefit References Chinnock B, Hendey GW, Minnigan H, Butler J, Afarian H. Clinical impression and ascites appearance do not rule out bacterial peritonitis. J Emerg Med. 2013 May;44(5):903-9. doi: 10.1016/j.jemermed.2012.07.086. Epub 2013 Mar 7. Pericleous M, Sarnowski A, Moore A, Fijten R, Zaman M. The clinical management of abdominal ascites, spontaneous bacterial peritonitis and hepatorenal syndrome: a review of current guidelines and recommendations. Eur J Gastroenterol Hepatol. 2016 Mar;28(3):e10-8. doi: 10.1097/MEG.0000000000000548. Chavez-Tapia NC, Barrientos-Gutierrez T, Tellez-Avila F, Soares-Weiser K, Mendez-Sanchez N, Gluud C, Uribe M.Meta-analysis: antibiotic prophylaxis for cirrhotic patients with upper gastrointestinal bleeding - an updated Cochrane review. Aliment Pharmacol Ther. 2011 Sep;34(5):509-18. doi: 10.1111/j.1365-2036.2011.04746.x. Epub 2011 Jun 27. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 527: Knee Dislocations
Contributor: Erik Verzemnieks, MD Educational Pearls: Knee dislocations are most common in high energy trauma, such as a motor vehicle accident The knee may appear grossly normal on initial inspection since dislocations can spontaneously reduce - Look for such findings as hemarthrosis, instability, or ecchymosis, as clues to an occult dislocation. Knee dislocations are often associated with damage to the popliteal artery that runs behind the knee. Assess for pulse deficit on exam. If you are concerned - use the ankle-brachial index (normal >0.9). If the ABI is abnormal, evaluate with CT angiogram and a vascular surgery consult. References Mills WJ, Barei DP, McNair P. The value of the ankle-brachial index for diagnosing arterial injury after knee dislocation: a prospective study. J Trauma. 2004 Jun;56(6):1261-5. Steele HL, Singh A. Vascular injury after occult knee dislocation presenting as compartment syndrome. J Emerg Med 2012; 42:271. Sillanpää PJ, Kannus P, Niemi ST, et al. Incidence of knee dislocation and concomitant vascular injury requiring surgery: a nationwide study. J Trauma Acute Care Surg 2014; 76:715. Summarized and written by myself

Podcast 526: Desmopressin for Intracranial Hemorrhage
Contributor: Charleen Melton, PharmD Educational Pearls: Desmopressin (DDAVP) is an analogue of anti-diuretic hormone (ADH) that has been used for the treatment of intracranial hemorrhage. It works by increasing the release of Von Willebrand factor, helping to stabilize clots. The use of DDAVP for intracranial hemorrhage in patients on antiplatelet agents (mainly Aspirin and Plavix) was recently reviewed In this retrospective review, they found an 88% decreased likelihood of hemorrhage expansion, in those who received DDAVP, compared to those who did not. Furthermore, they found no significant increase in adverse effects like hyponatremia or thrombosis However, no difference in mortality or neurological status was found DDAVP for intracranial hemorrhage in the setting of antiplatelet agents may be safe and reduce the expansion of intracranial bleeds but not change important patient outcomes References Feldman EA et al. Retrospective assessment of desmopressin effectiveness and safety in patients with antiplatelet-associated intracranial hemorrhage. Crit Care Med 2019 Sep 24; [e-pub] Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD
Podcast 525: Enjoyable Epistaxis?
Contributor: Jared Scott, MD Educational Pearls: The ED is full of painful procedures. One of the most commonly dreaded procedures is nasal packing for epistaxis, as it is quite uncomfortable for the patient. A recent study compared TXA with compression, saline with compression, and traditional nasal packing for the treatment of epistaxis. Hemostasis was achieved in 91% with TXA and compression, 93% with nasal packing, and 71% with saline and compression. There was no statistically significant difference between the packing and TXA groups. Furthermore, there was no difference in rates of rebleeding between the TXA and packing groups. However, 15% of nasal packing patients demanded removal of the packing due to pain. Consider TXA (on gauze or atomized) for your next patient with epistaxis! References Akkan, Sedat et al.. Evaluating Effectiveness of Nasal Compression With Tranexamic Acid Compared With Simple Nasal Compression and Merocel Packing: A Randomized Controlled Trial. Annals of Emergency Medicine, Volume 74, Issue 1, 72 - 78 Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 524: Bacterial Endocarditis
Contributor: Sue Chilton, MD Educational Pearls: More intracardiac devices and injection drug abuse are thought to be increasing incidence of endocarditis Classic signs of endocarditis have included: Osler nodes (painful hemorrhagic lesions on hands and feet), Janeway lesions (painless hemorrhagic lesions on the hands and feet), and splinter hemorrhages in the nail beds Other classic findings like fever and murmur are variable More non-specific symptoms can include flu-like symptoms Patients who inject drugs are at higher risk for this diagnosis References Pant S, Patel NJ, Deshmukh A, Golwala H, Patel N, Badheka A, Hirsch GA, Mehta JL Trends in infective endocarditis incidence, microbiology, and valve replacement in the United States from 2000 to 2011. J Am Coll Cardiol. 2015;65(19):2070. Infective endocarditis. Cahill TJ, Prendergast BD Lancet. 2016;387(10021):882. Epub 2015 Sep 1. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 523: A Dizzying Diagnosis
Contributor: Don Stader, MD Educational Pearls: It can be difficult to distinguish between central and peripheral causes of vertigo. Cerebellar stroke should be considered with any dizzy patient. Signs and symptoms that suggest stroke as the cause of vertigo include: ataxia, cranial nerve deficits, and rapid onset of symptoms When cerebellar stroke is being considered, MRI is the imaging modality of choice since CT does not adequately visualize the posterior fossa. References Kim J, Lee H. Vertigo due to posterior circulation stroke. Semin Neurol. 2013 Jul;33(3):179-84. doi: 10.1055/s-0033-1354600. Epub 2013 Sep 21.

UnfilterED #3: Dr. Katie Bakes & Dr. Pete Bakes
Husband and wife Pete and Katie Bakes, both emergency physicians in the Denver-Metro area, reflect on their upbringings, the many lessons learned over their twenty year careers, and how they've evolved as physicians and as a couple in this very special episode of UnfilterED. Time Stamps: 00:25 - Intros 03:05 - How did you two meet? 08:20 - (P) How have you seen Katie develop and change over the course of her medical career? 12:00 - (K) As a young woman, how did you balance your professional aspirations with your desire to start a family? 17:04 - (K) How have you seen Pete develop and change over the course of his medical career? 21:41 - Fostering and maintaining empathy over the course of a medical career 33:55 - How has medicine impacted the way you raise your children? 38:55 - Pete's experience as a 1st generation American 53:04 - How medicine has shaped Katie's faith and spirituality 1:00:24 - What is the purpose of suffering? 1:05:02 - Community vs. Academic medicine 1:09:40 - "The Award Winning Dr. Bakes" 1:12:40 - Extra-Clinical Pursuits Intro Music: Backbay Lounge Kevin MacLeod (incompetech.com) Licensed under Creative Commons: By Attribution 3.0 License http://creativecommons.org/licenses/by/3.0/

Podcast 522: e-Cigarette and Vaping Related Lung Injury
Contributor: John Winkler, MD Educational Pearls: Vaping-related lung injury initially presents with flu-like symptoms and can progress to respiratory failure requiring aggressive resuscitation including ECMO It is thought to be related to the contents of homemade vaping fluid, mostly in THC-containing products ("brands" include DankVapes, PaxPen) Ask patients with vague constitutional or respiratory symptoms about their vape use References What are the respiratory effects of e-cigarettes? Gotts JE, Jordt SE, McConnell R, Tarran R BMJ. 2019;366:l5275. Epub 2019 Sep 30. Pulmonary Illness Related to E-Cigarette Use in Illinois and Wisconsin - Preliminary Report.Layden JE, Ghinai I, Pray I, Kimball A, Layer M, Tenforde M, Navon L, Hoots B, Salvatore PP, Elderbrook M, Haupt T, Kanne J, Patel MT, Saathoff-Huber L, King BA, Schier JG, Mikosz CA, Meiman J N Engl J Med. 2019; Vaping-Associated Acute Lung Injury: A Case Series. Triantafyllou GA, Tiberio PJ, Zou RH, Lamberty PE, Lynch MJ, Kreit JW, Gladwin MT, Morris A, Chiarchiaro J. Am J Respir Crit Care Med. 2019; Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 521: Traumatic Hyphema
Author: Jared Scott, MD Educational Pearls: A hyphema is blood in the anterior chamber of the eye, typically caused by trauma While there is a spectrum of disease, blurred vision and eye pain are common presenting complaints after direct trauma to the eye Hyphema are graded between Grade 1 and Grade 5, depending on the amount of blood in the anterior chamber. Higher grades are associated with worse outcomes and more complications Other important diagnoses to consider include globe rupture and retrobulbar hematoma Complications of a hyphema can include glaucoma and vision loss References Brandt MT, Haug RH.Traumatic hyphema: a comprehensive review. J Oral Maxillofac Surg. 2001 Dec;59(12):1462-70. Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

Podcast 520: Approach to the arresting patient
Contributor: Peter Bakes, MD Educational Pearls: Peri-arrest patients present a particular challenge to ED providers, as the differential is broad and time is critical The differential for near cardiac arrest includes the "H's and T's", just as in true cardiac arrest The 6 H's include: hypoxia, hypo/hyperkalemia, hypovolemia (including shock states), hydrogen (acidosis), hypothermia The 6 T's include: tension pneumothorax, cardiac tamponade, thrombus (PE/MI), toxins, trauma Use your history skills to narrow down this list (i.e renal failure leads to hyperkalemia, trauma leads to tension pneumothorax or tamponade) Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD

CBHW Summit: The Cycle of Drug-Related Stigma - Implications for the Opioid Crisis
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Michael Miller, Strategic Initiatives Coordinator, Jefferson County Public Health

CBHW Summit: A Strategic Framework for Addiction Medicine
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributors: Judith Shlay, MD, MSPH, Associate Director, Denver Public Health, and Brooke Bender, MPH, Center for Addiction Medicine Planner, Denver Health

CBHW Summit: Safe Prescribing 101/201
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Christopher Urbina, MD, MPH, Colorado Consortium for Prescription Drug Abuse Prevention

CBHW Summit: Male Mental Health - A Crisis in Public Health
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Jason Vitello, MSW, Behavioral Health Coordinator, Denver Public Health/CPHA

CBHW Summit: Children's Mental Health
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributors: Sarah Davidon, EdD, Director of Research & Child and Adolescent Strategy, Mental Health Colorado, and Sarah Younggren, LCSW, Child & Adolescent Specialist, Mental Health Colorado

CBHW Summit: Positive Psychology and Well-Being
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Carl Clark, MD, President & Chief Executive Officer, Mental Health Center of Denver

CBHW Summit: Words Matter - How Language Can Shift Public Thinking
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Karen Prestia, MBA, Director, Marketing & Communications, Mental Health Center of Denver

CBHW Summit: Integrated Substance Use, Family Systems, and Culturally Responsive Treatment in Community Mental Health Settings
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributors: Allison Miller, LCSW, LAC, Program Manager of Child and Family Outpatient Services, Mental Health Center of Denver, and Jon Roberts, LCSW, CAC II, Licensed Mental Health Therapist, Mental Health Center of Denver

CBHW Summit: Substance Use During the Perinatal Period
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributors: Tracy Vozar, Ph.D., Director of the Infant and Early Childhood Mental Health Specialty, and Jennifer M. Tippett, Psy.D., Director of the Substance Use Disorder Specialty, both at the University of Denver's Graduate School for Professional Psychology

CBHW Summit: Strategies for Remaining Adaptive and Agile in Response to the Dynamic Issue of Substance (Mis)use
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributors: Marion Rorke, MPH, Substance Use Resource Coordinator, City and County of Denver, and Maggie Kauffman, MPH, Health Equity Data Analyst, City and County of Denver, and Jean Finn, RN, Substance Misuse Manager, City and County of Denver

CBHW Summit: Project Colorado Opioid Synergy
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributors: Lesley Brooks, MD, Chief Medical Officer, Sunrise Community Health Center; Medical Director – Quality, North Colorado Health Alliance, and Heather Ihrig, RN, CO-SLAW Program Director, North Colorado Health Alliance, and Meredith Silverstein, PhD, Sr. Research Associate, Butler Institute for Families, Graduate School of Social Work, University of Denver, and Kali Jefferson, MSW, Research Assistant, Butler Institute for Families, Graduate School of Social Work, University of Denver

CBHW Summit: Innovative and Interactive Approaches to Suicide Assessment and Safety Planning
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Khara Croswaite Brindle, MA, LPC, ACS, Croswaite Counseling, PLLC

CBHW Summit: Benzos - Boon or Blunder?
From DU's 1st annual Colorado Behavioral Health and Wellness Summit: Contributor: Steven Wright, MD, Colorado Consortium for Prescription Drug Abuse Prevention

Podcast 519: Malaria Drug Resistance
Contributor: John Winkler Educational Pearls: There is increasing resistance to antimalarial drugs, especially in P. falciparum. This trend started with chloroquine, but is now spreading to the other first-line drugs. Resistant strains have been identified in Cambodia and Thailand 220 million people were infected last year The best treatment of malaria is prevention from bites - DEET and permethrin are typical effective options. Permethrin may be applied to clothing items before travel, and will last through 6-8 wash cycles. While malaria is rare in the US, it should be considered in those having recently travelled References Hamilton WL, Amato R, van der Pluijm RW, et al. Evolution and expansion of multidrug-resistant malaria in southeast Asia: a genomic epidemiology study. Lancet Infect Dis. 2019;19(9):943–951. doi:10.1016/S1473-3099(19)30392-5 Summarized by Will Dewispelaere, MS4 | Edited by Erik Verzemnieks, MD