
FOAMfrat Podcast
101 episodes — Page 1 of 3
Podcast 192 - Salicylate Toxicity Management w/ Dr. Brookeman & Nicholas Henchal
Podcast 191 - Sepsis Update w/ Kevin Collopy
What does sepsis management look like for EMS? Tyler and Kevin Collopy break down the current state of sepsis care, including EMS recognition, hospital sepsis bundles, fluid strategies, vasopressor use, lactate trends, and the debate around prehospital antibiotics. The conversation focuses on practical decision-making and why identifying septic shock early can change outcomes long before the patient reaches the hospital.
Podcast 190 - Intubation Triggers w/ Nicole Hooser
"GCS less than 8, intubate." We've all heard it. Many of us were taught it. In this episode of the FOAMfrat Podcast, Tyler and FOAMfrat educator Nicole Hooser examine one of the most repeated airway phrases in EMS and why it may be doing more harm than good. From the origins of the "less than 8" mindset in GCS to the real-world complexity of airway decision-making, this conversation examines what actually matters when deciding whether to take a patient's airway. They discuss: • Why a GCS of 8 is not a magic number • The math behind GCS scoring combinations and why 8 carries so much variability • Airway protection versus airway reflexes • Resuscitation before intubation • The momentum problem once an RSI has been initiated • When hesitation is appropriate • When decisive action is necessary • Flight-specific pressures and transport considerations • Sedation versus full RSI • Reversible causes of altered mental status you cannot miss Nicole shares real-world flight cases, including moments of disagreement with partners and the professional growth that follows those cases. The episode also explores how experience, bias, fear, and pattern recognition shape airway decisions. If you've ever wondered whether you truly needed to intubate a patient, this episode challenges reflexive thinking and reinforces a more deliberate approach. Guest: Nicole Hooser Listen in and weigh in on the discussion.
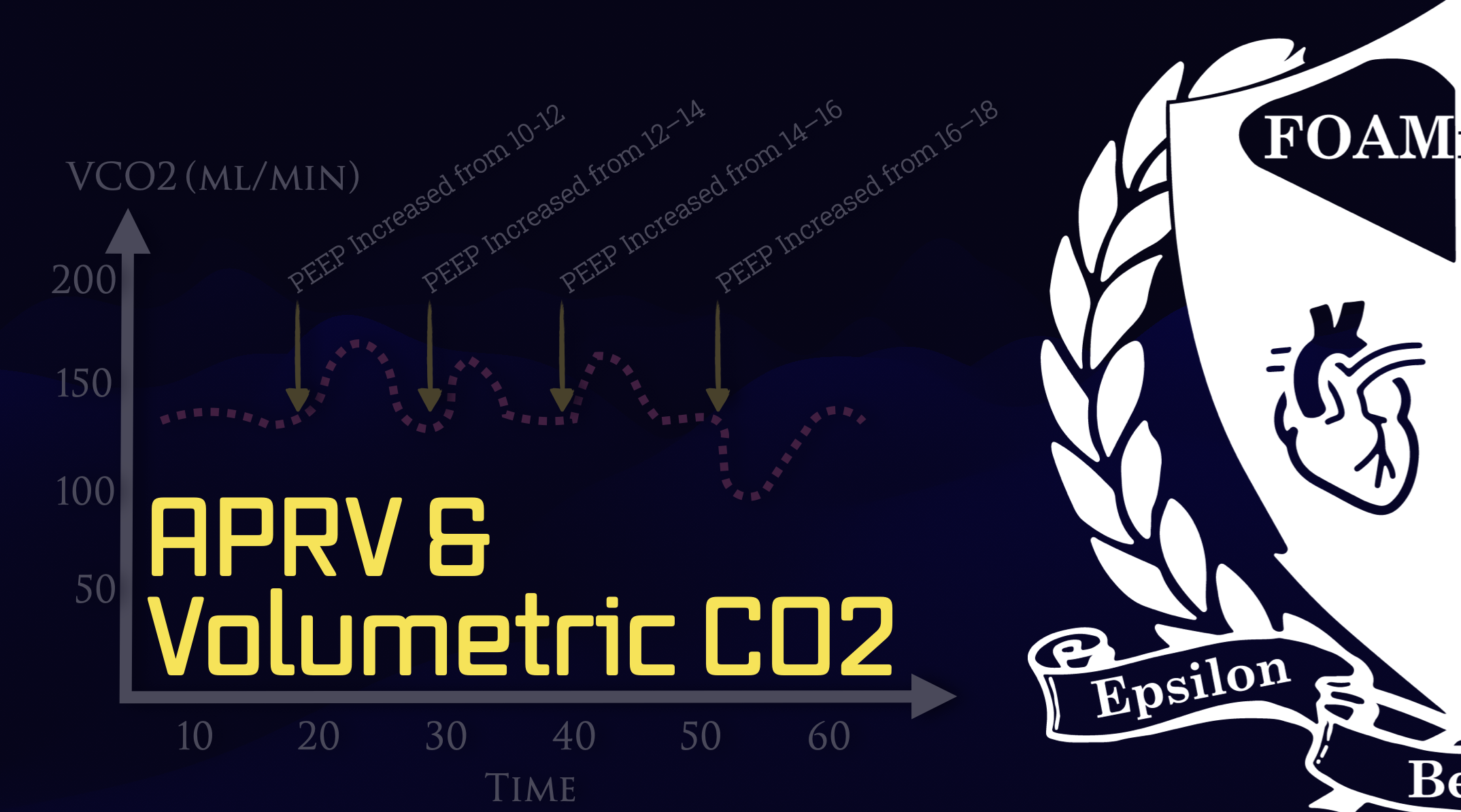
Podcast 189 - APRV & Volumetric CO2 w/ Joe Hylton
In this episode of the FOAMfrat Podcast, we sit down with Joe Hylton, one of the go-to ventilator educators in critical care transport, to break down APRV in a way that actually makes sense. We move beyond surface level explanations and get into how APRV really works, why it is so effective for ARDS and severe hypoxemia, and how volumetric capnography can give you real-time physiologic feedback when titrating mean airway pressure and PEEP. This is not a "set it and forget it" APRV discussion. We dig into the mechanics, the physiology, and the bedside decision making that matters in transport and critical care environments. Topics covered in this episode: • How APRV differs from conventional pressure control ventilation • Why mean airway pressure is the real driver of recruitment • Using flow curves and time constants instead of guesswork • Volumetric CO₂ vs end-tidal CO₂ and why the difference matters • Identifying optimal recruitment and overdistension in real time • How VĊO₂ trends can guide PEEP and pressure adjustments • APRV pitfalls, misconceptions, and when paralysis may still make sense • Practical APRV setup on Hamilton ventilators for transport teams If APRV has ever felt like ventilator voodoo, this episode pulls the curtain back and ties the mechanical settings to what is actually happening at the alveolar and capillary level. Joe brings deep experience from working with Hamilton Medical systems, and the discussion is framed through real-world transport and ICU decision making, including insights relevant to teams like Life Link III and other critical care programs. This episode is ideal for: • Flight paramedics and critical care transport clinicians • ICU nurses and respiratory therapists • Medical directors and educators • Anyone who wants to understand APRV beyond memorized settings 🎧 Listen, learn, and rethink how you approach lung recruitment. Subscribe for more high-yield critical care and EMS education from FOAMfrat.

Podcast 188 - Sodium Nitrite Ingestion & Methemoglobinemia w/ Dr. Brookeman
In this episode of the FOAMfrat Podcast, Dr. Harrison Brookeman joins the discussion to examine methemoglobinemia and the emerging prehospital threat of sodium nitrite ingestion. Often viewed as a rare toxicology concept, this condition is appearing more frequently and can progress rapidly with devastating consequences if it is not recognized early. The episode focuses on what matters most to EMS clinicians in the field: the physiology of methemoglobinemia, why these patients appear profoundly hypoxic despite adequate ventilation, and the classic clue: a pulse oximetry reading that remains fixed around 85 percent regardless of oxygen delivery. The conversation also addresses iatrogenic causes such as benzocaine exposure, expected mental status changes, and why oxygen alone does not correct the problem. Emphasis is placed on prehospital decision-making, including early involvement with poison control, transport destination considerations, and the importance of ensuring these patients are taken to the right facility the first time. This episode is intended to sharpen recognition, improve pattern awareness, and prepare providers for a call that does not follow typical respiratory failure patterns.
Podcast 187 - Dynamic PEEP? | Ventilation Strategies for Metabolic Acidosis w/ Melody Bishop, RRT
A little over a year ago, I made a short reel discussing ventilating a patient in a severe metabolic acidosis. In the video, I mentioned that minimal to no PEEP might be appropriate. Not because the patient doesn't need PEEP, but because the shortened cycle time at higher respiratory rates can unintentionally generate dynamic PEEP on its own. But what if it was intentional? What if the presence of a wider pressure when the ventilator switches into exhalation would cause the air to exit more rapidly? In this podcast, I discuss my thought process with respiratory therapist extraordinare, Melody Bishop @melodybishop_rt. She helps surface some definitions and distinctions to terms like air-trapping, Set PEEP, & auto-PEEP while we discuss ventilation strategies in metabolic acidosis. The blog below was what I had sent her before the podcast to get all my thoughts & illustrations down in writing. As always, please follow your local guidelines, and I hope you enjoy listening to the conversation.

Podcast 186 - Should we throw away our pelvic binders? w/ Dr John Lyng
Pelvic binders have long been considered a standard intervention in the management of suspected pelvic fractures in the prehospital setting. However, recent guidance from the National Association of EMS Physicians (NAEMSP) challenges some of the long-standing assumptions surrounding their use. In a recent FOAMfrat podcast episode, I spoke with Dr. John Lyng, editor-in-chief of the NAEMSP Trauma Compendium, to explore the evidence and rationale behind their newly released position statement on pelvic fracture management.
Podcast 185 - Eating Disorders w Hanna Thompson
In this episode, Tyler sits down with Hanna Thompson to discuss a critical yet often overlooked topic in EMS—eating disorders. Drawing from personal experience and clinical insight, they explore how these conditions present both medically and behaviorally, especially in prehospital and interfacility transport settings. They break down the subtle physical signs that EMS providers can look for—such as Russell's sign, lanugo, unexplained bradycardia, and electrolyte disturbances—and emphasize the importance of sensitive history taking. The conversation also dives into the dangers of refeeding syndrome, slow correction strategies, fluid choice, and the clinical significance of thiamine, magnesium, and phosphate replacement. What You'll Learn: How eating disorders can manifest in EMS calls Why you may be treating the consequences, not the disorder itself Red flags like bradycardia, lanugo, and Russell's sign How to handle refeeding syndrome safely Why dextrose, fluids, and electrolyte replacement should be approached cautiously The connection between electrolyte shifts and seizures or arrhythmias Key Takeaway: Patients with eating disorders are medically and psychologically fragile. In EMS, we often encounter them through the effects of the disorder—not the diagnosis itself. Recognizing subtle clues and avoiding aggressive interventions could save a life. Resources Mentioned: Hannah's blog on EMS considerations in eating disorders Data on post-COVID spikes in eating disorder incidence Guidelines for electrolyte correction and refeeding syndrome Disclaimer: This podcast is for educational purposes only and not a substitute for clinical protocols or medical direction. Always consult your agency's guidelines and medical control.
Podcast 184 - Diastolic Augmentation w/ Brian Cress
In this episode, Tyler Christifulli sits down with cardiac perfusionist Brian Cress to dig into the physiology of coronary perfusion, the mechanics of the intra-aortic balloon pump (IABP), and the clinical finesse of diastolic augmentation. Whether you're just starting to encounter balloon pumps or want to sharpen your transport strategy, this discussion is packed with visual metaphors, waveform analysis, and real-world pearls.
Podcast 183 - Cardiac Ultrasound w/ Dr. Weimersheimer
In this conversation, Dr. Peter Weimersheimer discusses various techniques and tips for performing cardiac ultrasound in emergency medicine. He emphasizes the importance of understanding probe movements such as sliding, fanning, and rocking to optimize cardiac views. The discussion also covers troubleshooting common challenges in cardiac imaging, the critical role of gel in obtaining clear images, and the transition between different cardiac views. Dr. Weimersheimer emphasizes the importance of identifying cardiac pathologies through ultrasound and shares techniques for obtaining the apical four-chamber view. The conversation concludes with insights into the impact of ultrasound on patient care and decision-making in emergency situations. In this conversation, Dr. Peter Weimersheimer shares his expertise on cardiac ultrasound techniques, with a focus on the apical four-chamber view and the importance of understanding ventricular shape and function. He discusses practical tips for navigating ultrasound views in critical situations, optimizing imaging techniques, and utilizing patient physiology to enhance imaging quality. The conversation also covers the interpretation of right ventricular size in cardiac arrest and differentiating between the inferior vena cava (IVC) and aorta during ultrasound imaging.
Podcast 182 - AHORA Spanish Stroke Assessment
Stroke assessment tools like BEFAST are crucial for swiftly identifying symptoms and expediting treatment. However, language barriers can hinder prompt care for non-English speakers, particularly in the Hispanic community. Developed through a collaborative effort, AHORA adapts the traditional stroke assessment to be culturally and linguistically appropriate for the Spanish-speaking population. Designing Ahora The need for a specific tool became apparent when traditional tools like BEFAST were found to be ineffective for those who did not speak English. After discarding the complex "Rapido," Banerjee's team crafted Ahora, including Marcia Wilson, MD, and Remley Crowe, PhD. This tool was made to mirror BEFAST but is simplified for practical use within the Spanish-speaking population.
Podcast 181 - Discrepancies in Testing & Treatment
Does medicine have dangerous side effects for women? Are the "normal" values we have set for diagnostics possibly endangering specific populations? In this episode of the FOAMfrat podcast, Tyler sits down with Dr.Alyson McGregor, emergency physician and author of Sex Matters, and Tim Redding, EMS educator and lecturer, to discuss the discrepancies in medical testing, diagnosis, and treatment between male and female patients. Dr. McGregor shares her journey of discovering gender bias in medicine, particularly how women's symptoms are often dismissed or mislabeled as psychiatric in nature. The discussion explores how male-centric research has shaped clinical guidelines, leading to underdiagnosis and undertreatment of women across a wide range of conditions—from heart attacks to strokes and even pain management.

Podcast 180 - MCI Collaboration w/ ATCEMS & Travis County Star Flight
In this episode of the FOAMfrat podcast, join as we discuss mass casualty management with Chief Robert Luckritz of Austin Travis County EMS and Justin Soulier from Travis County Star Flight. Explore the strategies and challenges in mass casualty responses in one of the fastest-growing urban areas in the U.S.

Podcast 179 - Your First 5 Minutes of an MCI w/ Rommie Duckworth
Join Rommie Duckworth and FOAMfrat as we discuss the mental framing and big-picture thought process behind the first five minutes of any mass casualty incident (MCI). Rommie Duckworth, a fire captain and shift commander, is a wealth of knowledge on this topic and speaks globally to prepare emergency responders for these events.
Podcast 178 - ECPR Eligibility and Preparation w/ Alec Wilcox
In this episode, Alec Wilcox & I discuss ECPR eligibility & preparation. ECPR, or extracorporeal cardiopulmonary resuscitation, involves taking a patient in cardiac arrest, sucking blood from their venous system, oxygenating it externally, and then pumping it back into their arterial system. This procedure helps maintain blood circulation and oxygen delivery during cardiac arrest, serving as a bridge to further therapy.
Podcast 177 - Implementing Ultrasound w/ Allen Wolfe
The integration of point-of-care ultrasound (POCUS) is transforming emergency medical services (EMS) by enhancing diagnostic capabilities and improving accuracy in answering important clinical questions. Recently, I had the opportunity to discuss this topic extensively with Allen Wolfe, the Senior Director of Education at Life Link III. A significant challenge in incorporating ultrasound technology within EMS has been overcoming initial barriers to adoption. Many programs, burdened by cost concerns and technological intimidation, have historically relegated ultrasound units to the back shelves. However, as Allen outlined, strategic changes in accessibility and training can dramatically alter this landscape.
Podcast 176 - Pediatric TBI Protcol w/ Dr. Banerjee
In this episode, Dr Banerjee and I discuss a new traumatic brain injury (TBI) protocol his department is trialing for pediatric patients with moderate to severe TBI in collaboration with Arnold Palmer Hospital. This protocol involves administering Keppra and 3% saline in the pre-hospital setting.

Podcast 175 - The Things We Do w/ PulmCCM
Matt Hoffman is the editor-in-chief of PulmCCM, a blog that frequently updates its readers on evidence and best practices in critical care medicine. I have always wondered how our work in the field affects a patient's care downstream. Do pulmonologists ever sigh to themselves and think, "God, I wish paramedics would just start/stop doing ____________?" It turns out that this is not the case, but the discussion was super interesting, and I thank Dr. Hoffman for coming to the show.
Podcast 174 - "I Rolled My Ambulance" Interview w/ Kyle Rice
In this episode of FOAMfrat, Tyler speaks with paramedic Kyle Rice to discuss a deeply personal and eye-opening experience—rolling his ambulance after running a red light. Kyle shares the lessons he learned about complacency, crew resource management, and the often-overlooked dangers of driving with lights and sirens. Together, they explore how EMS providers can stay vigilant behind the wheel, adopt safer driving practices, and shift their mindset when responding to emergencies. If you're an EMS provider, this episode is a must-listen for understanding the real-life risks of complacency and how to prevent accidents.
Podcast 173 - Rethinking Lights & Sirens w/ Jeff Jarvis & Jonathon Jenkins
In this episode, I sit down with Dr. Jeffrey Jarvis, author of a fascinating paper on the impact of lights and siren (L&S) use in EMS responses. If you're like most of us, when you hear those blaring sirens and see flashing lights, you think, "Wow, someone's really in trouble!" But the truth, according to Dr. Jarvis' study, might surprise you.
Podcast 172- Hamilton T1 Hacks & Strategies w/ Joe Hylton
In this podcast, we discuss the nuances and strategy of the T1 ventilator with RRT, Joe Hylton. Whether you're a paramedic or a healthcare professional involved in critical care transport, understanding the nuances of this advanced ventilator is essential to safe and effective patient transport. We break down the pressure-controlled ventilation with volume adaptive options and offer practical guidance on managing obstructive lung conditions like asthma during transport. Plus, we cover essential troubleshooting techniques to help you address common issues when things don't go as planned.

Podcast 171 - Thoracic Dissection Goals w/ Alex Greene
Thoracic dissections are surgical emergencies that require precise temporizing measures until surgery can be performed. In this session, participants will gain critical knowledge on recognizing key symptoms such as ripping back pain and unequal pulses, indicative of thoracic dissections. The discussion will focus on anti-impulse therapy, emphasizing using beta-blockers like esmolol and calcium channel blockers like nicardipine to control blood pressure and prevent further damage. Pain management strategies and the selective use of nitroprusside will also be explored. The class will address the unique challenges of managing blood pressure in prehospital settings, stressing the importance of a well-prepared plan.

Podcast 170 - Finger Thoracostomy w/ Dr. Cynthia Griffin
In this conversation, Tyler and Dr. Cynthia Griffin discuss the finger thoracostomy procedure. They cover topics such as when to choose finger thoracostomy over needle decompression, the equipment needed for the procedure, the technique for performing the procedure, and potential complications and tips for success. They also touch on the use of chest tubes and the management of tension physiology. Overall, the conversation provides a comprehensive overview of the finger thoracostomy procedure.
Podcast 169 - EVD Transport Logistics w/ Alaina Martini
Alaina Martini, a flight nurse at Allegheny Life Flight, shares her expertise on transporting patients with external ventricular drains (EVDs). She explains the indications for EVD insertion, such as aneurysmal subarachnoid hemorrhage and obstructive hydrocephalus. Alaina discusses the importance of assessing the color and texture of the cerebrospinal fluid (CSF) to detect changes and potential rebleeding. She also explains the process of inserting the EVD and how it is guided by CT scans to avoid damaging important brain tissue. Alaina emphasizes the need to know if the aneurysm is secure before adjusting the EVD drain level, as opening it too low can increase the risk of rebleeding. She also discusses the use of hypertonic saline and osmotic therapy to manage increased intracranial pressure. Tyler and Alaina discuss various aspects of managing patients with external ventricular drains (EVDs) during transport in this conversation. They cover topics such as the clamping of EVDs, positioning the patient's head, troubleshooting common issues, and securing the EVD during transport. Alaina provides insights and recommendations based on her experience as a neurocritical care nurse.

Podcast 168 - Procedure Preppers (Needle Decompression) w/ Dr. Aho
Dr. John Aho discusses needle decompression and the procedure's indications, techniques, and potential pitfalls. He emphasizes the importance of high clinical suspicion and the limitations of external signs in diagnosing tension pneumothorax. The conversation also covers the choice of needle insertion sites, the use of ultrasound, and the need for proper training and practice. Dr. Aho provides insights into the anatomical considerations and common mistakes made during needle decompression. He also explores the possibility of instant feedback to confirm successful decompression. The conversation discusses the problem of needle decompression failure rates and the need for a reliable indicator of successful decompression. The guest introduced the Cap-No-Spot, a device that uses colorimetric indicator paper to detect CO2 and determine if a needle decompression procedure was successful. The device has been shown to have higher sensitivity and specificity than human judgment. The conversation also touches on the importance of proper training and the device's potential applications beyond pneumothorax detection.

Podcast 167 - Placenta Previa w- Demi Wilkes
An iceberg typically shows only 10% of its mass above water. To appreciate the other 90%, you need to dive deep. That's precisely what we're doing in this series—discovering the deeper knowledge about obstetric topics. These topics can be massive, and much of the information is below the 'surface-level' knowledge that EMS is presented with. In this episode, Demi Wilkes & I will discuss Placenta Previa and the closely associated Placenta Accrete Spectrum.

Podcast 166 - Transcutaneous Pacing & False Capture
The conversation is about a paper on false electrical capture and pre-hospital transcutaneous pacing by paramedics. The guests, Tom Boutilet, Josh Kimbrell, and Judah Kreinbrook, discuss their research findings and the implications for paramedics. They conducted a retrospective study and found that paramedics often mistakenly believe they have electrical capture when they do not. They emphasize the importance of confirming electrical capture before assuming mechanical capture. They also discuss the challenges of pulse palpation and the need for more rigorous research in EMS and ED settings. The conversation discusses the challenges and considerations in transcutaneous pacing, specifically focusing on the verification of mechanical capture. The speakers explore the use of various methods to confirm mechanical capture, such as feeling for a pulse, using pulse oximetry, and utilizing ultrasound. They also discuss the difficulty of accurately assessing mechanical capture and the potential for false electrical capture. The conversation concludes with a discussion on the transfer of pacing from one device to another and the importance of verifying capture during the process.

Podcast 165 - Should Pressors Have A Max Dose?
In this episode we discuss whether the concept of having a "max dose" of your pressor has any evidence or physiological backing. Joining me in this discussion are Dan Rauh, Shane O'Donnell, and Shad Ruby.
Podcast 164 - Suicidal Ideation w/ James Boomhower
How do you talk to a patient experiencing suicidal ideation? What if you're the one having these thoughts? We're interviewing James Boomhower from Stay Fit 4 Duty in this episode. We discuss suicidal ideation, therapeutic communication, and verbal de-escalation.
Podcast 163 - What Can We Learn From A Ketamine Infusion Clinic? w/ Chris Carlstrom
Chris Carlstrom is a flight nurse at Life Link III and also works part-time at a ketamine infusion clinic. We've had some interesting conversations on shift regarding his experiences with ketamine in the clinic versus emergency medicine and I finally was able to get one of these conversations recorded for the podcast. Enjoy Podcast 163 - What Can We Learn From A Ketamine Infusion Clinic? w/ Chris Carlstrom.
Podcast 162 - Multimodal Pain Management w/ Shane O' Donnell
When I became a paramedic, being able to provide pain management was one of the "new interventions" that I looked forward to most. As an EMT, I remember countless times I was without ALS resources and had to watch a patient suffering in pain until we got to the hospital. Trying to obtain any history or perform an assessment on someone writhing in pain can be nearly impossible. As a BLS provider, I would attempt non-pharmacological ways to relieve pain, such as ice packs, warm packs, elevating extremities, and sometimes simply trying to distract them with conversation. While these methods should not be discounted, I will never forget the first time I could provide pain medication to an elderly woman who fell and fractured her hip. I started an IV right there on the floor of the assisted living facility, administered some fentanyl, and comfortably got her to the stretcher. Analgesia did not save this lady's life. Still, it did make her trip to the hospital a little more comfortable and allowed me to obtain an accurate history, including the dizziness and dyspnea she felt before falling. Performing an adequate assessment and obtaining pertinent medical history can be difficult when a patient is experiencing intense pain. For this reason, pain should be managed to a level that allows for comfort & communication. Total pain relief is ideal but may not always be feasible, given hemodynamics and underlying causes. Check out this episode with Tyler & Shane as they discuss multimodal pain management strategies.
Podcast 161 - EMT Pharmacology
Taking on pharmacology in EMT school is a big hurdle. We wanted to write something that not only explained the basics of the medications but also helped bridge the gap between what EMTs are taught and what paramedics learn when they go back over these medications in paramedic pharmacology. Each chapter discusses how the medications work, why they're given for specific indications, and the logistics of medication administration! We've also included medication profiles, tips and tricks from experienced providers, and flashcards for each medication to help you hone your med knowledge base! In this book, we're coving: Oxygen Albuterol and Atrovent Epinephrine Aspirin Nitroglycerin Naloxone Oral Glucose Gel and Glucagon + Flashcards in the back! This book is for students, EMTs, and paramedics who want an in-depth review of EMT medications! You can download the book for free at foamfrat.com
Podcast 160 - Autism Communication w/ Joshua Chan & Matthew Yelton
I had the privilege to bring on two passionate fathers of children with Autism to help me better understand how to approach and communicate with a neuro-diverse child. This episode is chock-full of insight, tips, tricks, and logistics of approaching a child in the field with Autism. Josh Chan is a Life Link III flight paramedic/base lead and a Glenwood FD firefighter. Matthew Yelton is a flight paramedic/base lead for Mercy Flight Central and works as a fire captain at Constableville Ambulance Inc.

Podcast 159 - Close Encounters of the Infectious Kind w/ Dr. Hudson Garrett
EMS providers encounter various infectious diseases daily and need to know the routes of exposure, risks, and preventive measures to protect themselves and their families. In this episode, We talk with Dr. Hudson Garrett, an infectious disease expert with the medical college of Louisville University, to discuss the practical points of infectious disease for the everyday provider. Want CE for this episode? Sign up for FOAMfrat Studio and access 300+ hours of continuing education for EMS & Nursing. www.foamfrat.com
Podcast 158 - RSI Cocktail w/ Heavy Lies The Helmet
In this episode, Dan Rauh & Mike Boone from Heavy Lies The Helmet join me to hash out our workflows and drugs of choice for four particular scenarios you may come across. The combative head injury patient that needs to be intubated but has five firefighters holding them down and is actively trying to rip off his collar and IV. The septic hypotensive patient is no longer protecting their airway but also needs resuscitation prior to induction. The snoring head bleed with a BP of 220/140 The "almost dead, but needs a tube" population (induction med?)
Podcast 157 - Ventilation & Cardiac Arrest w/ Tom Bouthillet
Moments after the heart stops the entire circulatory system finally has a chance to bring venous and arterial pressures to equilibrium. Cardiac arrest resuscitation requires the provider to have a strong mental model of physiology and the logistics to carry out a series of interventions crucial to preserving life. This class will serve not as a routine basic life support model, but as a deeper understanding and framework to guide resuscitation during your next cardiac arrest.
Podcast 156 - Is using AI cheating? EMS and AI
AI will be integrated into everything we do in medicine, perhaps sooner than we think. It will help keep our patients safe, our providers informed, and our communications connected, and change how we think about how we care for patients (if implemented correctly). Systems like ChatGPT are only the beginning, and many companies are already working on or have already integrated with other healthcare specialties. We will see the same integration happen with EMS. While the response to this might be fear of losing our knowledge base, over-automating decision-making, cheating on tests and papers, and the like, we could adopt a very different outlook. We could view this as an opportunity to improve patient safety, offload menial work, automate documentation and communications, and always have an intelligent partner in our pockets we can bounce ideas off of. One day, we'll wonder how we ever lived without it.

Podcast 155 - Pattern Recognition vs. Autopilot w/ Shaylah Montgomery
In this episode, Tyler is joined by Shaylah Montgomery to discuss decision-making, human factors, and mental shortcuts utilizing pattern detection. Shaylah is a flight nurse and paramedic for Pafford Air One and a member of the FOAMfrat team.
Podcast 154 - ROSC Temp & Sedation w/ Dr. Leon Eydelman
0.9. When a patient is in shock, their volume of distribution changes, and peripheral blood flow is reduced. This means more blood is shunted to the brain,, and lower doses of sedation will give the agent therapeutic brain levels.","type":"unstyled","depth":0,"inlineStyleRanges":[],"entityRanges":[],"data":{}}],"entityMap":{},"VERSION":"9.3.6"}"> What aspects of temperature-targeted management are most important to EMS, and how should EMS guide sedation for the patient with a return of spontaneous circulation? Check out this interview w/ Dr. Leon Eydelman! The ROSC class referenced in this video can be found in FOAMfrat Studio! Highlights ROSC + FEVER = Bad. Trust a high temperature and question a low one. While most EMS agencies likely do not carry propofol, it is the most commonly used sedation medication in the ED because it washes out quickly and allows for neuro eval. Benzodiazepines are associated with higher rates of ICU delirium and complications. Running levophed to counteract the vasodilation aspect of propofol. Don't have propofol; hemodynamic-dosed ketamine is a good option as well. The sedation dose should be reduced when the shock index is > 0.9. When a patient is in shock, their volume of distribution changes, and peripheral blood flow is reduced. This means more blood is shunted to the brain,, and lower doses of sedation will give the agent therapeutic brain levels.
Podcast 153 - Pediatric Arrest w/ Dr. Banerjee
We just finished re-recording our pediatric arrest class in Studio and decided to play the unedited version of my discussion with Dr. Paul Banerjee. Banerjee is a prolific researcher and medical director in Florida with a particular emphasis on pediatric arrest. Check out the class in Studio for more information on the logistics.
Podcast 152 - CISM & Processing w/ Sam Henne
Sam Henne is the creator of Mind Over Medic and a co-worker of mine at Life Link III. In this episode, we discuss the components of critical incident stress and ways to reduce adrenaline during threat appraisal. Check out www.mindovermedic.com
Podcast 151 - Central Line Access for EMS w/ Austin Brook
EMS is well-trained in peripheral intravenous as well as intraosseous access. However, central lines remain off-limits for many clinicians in various response areas. If accessing these types of lines is allowed, it's usually permitted when the patient is (nearly) dead. This isn't very surprising since the scope of practice of the EMS clinician usually focuses on emergent treatments. Unless it's learned during a critical care class, little thought is typically given to topics like central, dialysis, and PICC lines in EMS. Why not?
Podcast 150 - Slishman Traction
Had the opportunity to talk with Dr. Sam Slishman, the inventor of the Slishman traction splint. We had a great conversation on the idea/concept of this splint, who to apply it on, and some additional questions, which we plan on having him back on to discuss.
Podcast 149 - P:F vs. A-a & Oxygenation Strategies
A-a gradient, a/A ratio, and P: F ratio - are all different views of the same item. These formulas do not have a complete view of oxygenation. Oxygenation is a huge topic, and there are more common values that we use: How well is the patient saturating? Is there dyspnea? How do the lungs sound (auscultation) or look (POCUS)? Where is the patient on the OHCD? What does the ABG show?
Podcast 148 - Crashing PE Logistics w/ Shane & Brian
I ran some specific decision points when treating the REALLY BAD massiVE pulmonary embolism patient by Shane & Brian from the FOAMfrat Team. This discussion really focuses on the logistics and ideas when you are trying to get the patient from A to B without having to do CPR.

Podcast 147 - NICU Q&A w/ Theresa Bowden
Theresa Bowden is a rockstar flight nurse who specializes in NICU transports. In this episode, you will listen in as Theresa explains anything and everything you have ever wondered about NICU interfacility transports. Topics include: Who gets prostaglandin? IO or IV catheter for UVC Cardiac vs. Respiratory Initial Vent Settings Get credit for this class by listening to it in FOAMfrat Studio.
Podcast 146 - IVC Assessment w/ Shane O'Donnell
Does IVC assessment have a role in pre-hospital ultrasound? This week we talk to one of the newest members of FOAMfrat, Shane O'Donnell.
Podcast 145 - Pediatric Bags
Do specialized pediatric jump bags alienate the pediatric population? They typically don't get used as much, and introducing a foreign bag into a low volume population may add to the stress of running a pediatric call anyway. In this episode, Sam & Tyler discuss the case against the pediatric jump bag.

Podcast 144 - VR & EMS Education
The FOAMfrat podcast is back in 2022 with a discussion on how virtual reality can be used in EMS education. We did our first VR class a few weeks ago and here's what we learned and what we plan to do with it!
Podcast 143 - Thyroid Disorders
The thyroid is a butterfly-shaped gland. But for some, it can be more like a bullet to the neck. The number of systems that our thyroid helps regulate truly is incredible, and an over or under-active thyroid can cause a whole host of acute and chronic issues. On the one hand, imagine a patient who has a thyroid history and is cold, weak, and has a depressed level of consciousness. Why is this occurring, and what's the diagnosis and treatment? On the other hand, imagine an anxious, hyperpyrexic patient in atrial fibrillation. Both patients have thyroid issues, but why do these patients present so differently? Let's see what happens when the scales tip either way for a few of the systems that the thyroid helps control!